 Ilinani RR, Shetty AP (2018) Fractures in ankylosed spines: Current concepts. Gao Q, Zhang Z, Shao T et al (2021) Predictor of surgical outcomes in ankylosing spondylitis cervical spinal fracture: an at least 2 years follow-up retrospective study. Īnwar F, Al-Khayer A, Joseph G et al (2011) Delayed presentation and diagnosis of cervical spine injuries in long-standing ankylosing spondylitis. Ĭhoi D (2015) Fractures in ankylosing disorders of the Spine: easy to miss and high risk of deterioration. 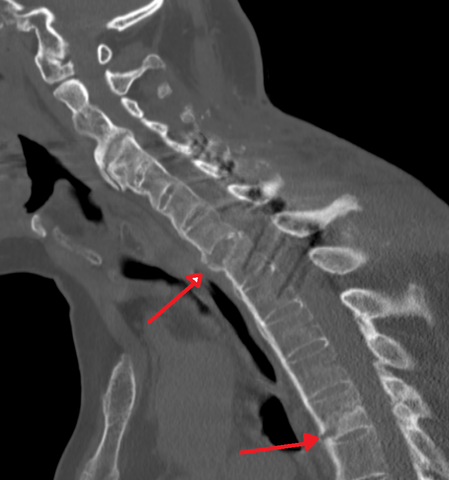
Reinhold M, Knop C, Kneitz C, Disch A (2018) Spine fractures in ankylosing diseases: recommendations of the spine section of the German society for orthopaedics and trauma (DGOU). Westerveld LA, Verlaan JJ, Oner FC (2009) Spinal fractures in patients with ankylosing spinal disorders: A systematic review of the literature on treatment, neurological status and complications. Ull C, Yilmaz E, Hoffmann MF et al (2021) Factors associated with major complications and mortality during hospitalization in patients with ankylosing spondylitis undergoing surgical management for a spine fracture. Lukasiewicz AM, Bohl DD, Varthi AG et al (2016) Spinal fracture in patients with ankylosing spondylitis: cohort definition distribution of injuries, and hospital outcomes. Robinson Y, Sandén B, Olerud C (2013) Increased occurrence of spinal fractures related to ankylosing spondylitis: A prospective 22-year cohort study in 17,764 patients from a national registry in Sweden. Prieto-Alhambra D, Muñoz-Ortego J, De Vries F et al (2015) Ankylosing spondylitis confers substantially increased risk of clinical spine fractures: a nationwide case-control study. Ĭaron T, Bransford R, Nguyen Q, et al (2010) Spine fractures in patients with ankylosing spinal disorders. Hartmann S, Tschugg A, Wipplinger C, Thomé C (2017) Analysis of the literature on cervical spine fractures in ankylosing spinal disorders. Von der Höh NH, Henkelmann J, Jarvers JS et al (2020) Magnetic resonance tomography for the early detection of occult fractures of the spinal column in patients with ankylosing spondylitis. Lazennec JY, d’Astorg H, Rousseau MA (2015) Cervical spine surgery in ankylosing spondylitis: Review and current concept. PhysicianĮtame AB, Than KD, Wang AC et al (2008) Surgical management of symptomatic cervical or cervicothoracic kyphosis due to ankylosing spondylitis. Golder V, Schachna L (2013) Ankylosing spondylitis: An update. Smith JA (2015) Update on ankylosing spondylitis: current concepts in pathogenesis. Surgical treatment is safe, and the posterior approach with long-segment fusion is the approach of choice in this group of patients. CT and MRI images are necessary to rule out cervical spine fractures in AS patients, especially to detect occult fractures. High suspicion of cervical spine fractures is necessary for patients with AS. The improvement was clinically significant (p = 0.01 and 0.00, respectively). VAS improved to 3 ± 1, and NDI improved to 14 ± 6 at the last postoperative visit. The mean postoperative follow-up was 46 ± 18 months. In 12 patients, the recovery was complete. Neurological improvement occurred in 20/27 patients. Postoperative Cobb angle improved to a mean of 17 ± 9 degrees. Intraoperative complications occurred in 9 patients (8.2%). The mean number of the fixed levels was 6 ± 2 levels. The surgical approach was dorsal in 59 patients (53.6%), combined in 45 patients (40.9%), and ventral in 6 patients (6,5%). Positioning and preparing of the patients on the operation table took a mean of 57 ± 28 min. The mean preoperative kyphosis angle was 48 ± 26° between C2 and C7. 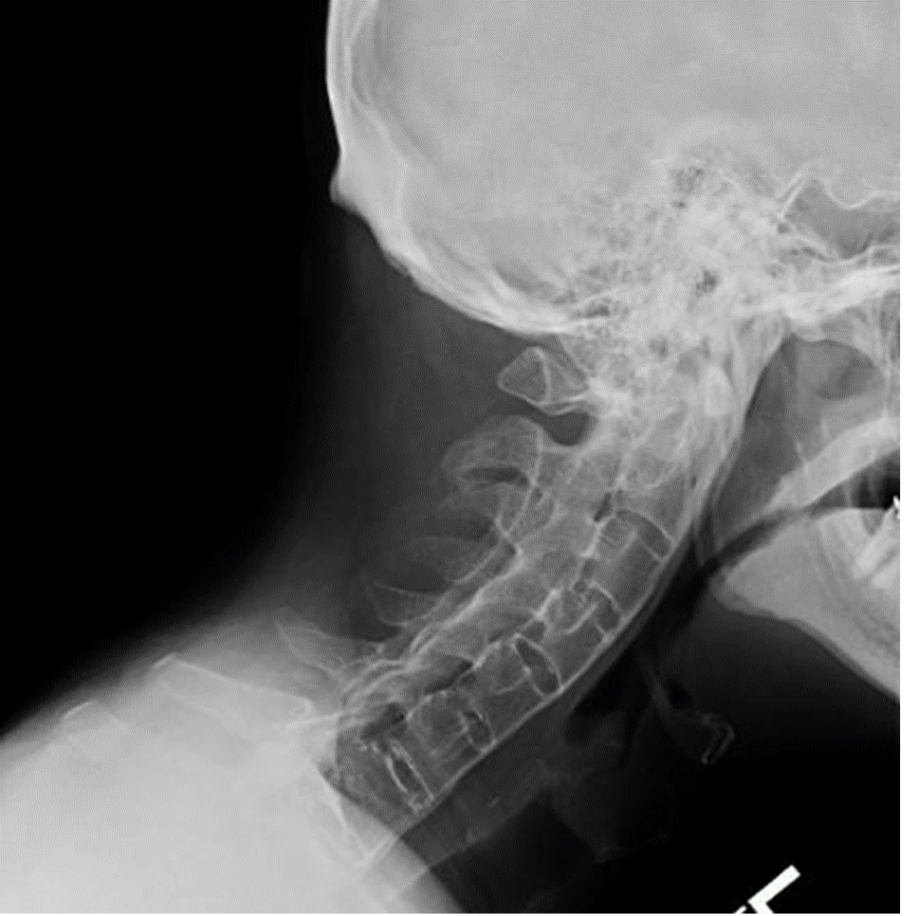
The VAS was 7 ± 1, and NDI was 34 ± 8 in the preoperative assessment. The most common fracture level was C6/7 in 63 patients (57.23%). Twenty-seven (24.6%) had a neurological deficit at admission. The clinical presentation was a pain in all patients. 
There was a history of mild trauma in 72 patients (65.4%). The mean time between trauma and surgery was 49 ± 42 days. One hundred ten patients (105 male/5 female) were included. Inclusion criteria were surgically treated AS with cervical spine fracture diagnosis (from C1 to Th3) and postoperative follow-up minimum of 12 months. Both spine centers have a standard database for all admitted patients. MethodsĪ retrospective analysis of prospectively collected data in two level-1 spine surgery centers was performed. In this work, a two-center study was performed to study the clinical presentation of cervical spine fractures in ankylosing spondylitis (AS) patients and assess the surgical management of these fractures. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
